X-ray
[table id=7 /]
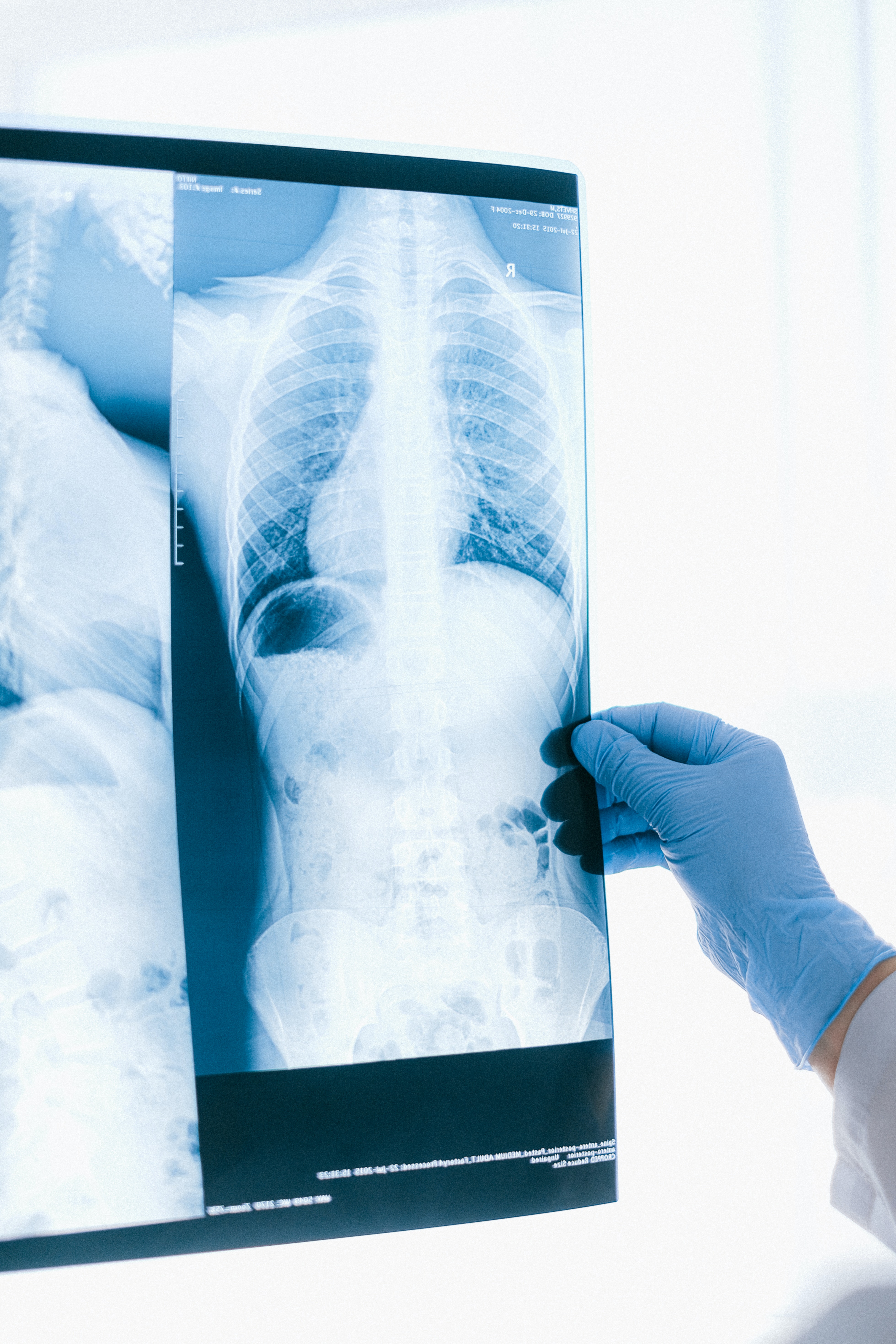
How to Read X-ray
Normal Chest X-ray

Mikael Häggström, CC0, via Wikimedia Commons

Mikael Häggström, CC0, via Wikimedia Commons
- A – Airway
- Ensure trachea is visible and in midline
- Trachea gets pushed away from abnormality, eg pleural effusion or tension pneumothorax
- Trachea gets pulled towards abnormality, eg atelectasis
- Trachea normally narrows at the vocal cords
- View the carina, angle should be between 60 –100 degrees
- Beware of things that may increase this angle, eg left atrial enlargement, lymph node enlargement and left upper lobe atelectasis
- Follow out both main stem bronchi
- Check for tubes, pacemaker, wires, lines foreign bodies etc
- If an endotracheal tube is in place, check the positioning, the distal tip of the tube should be 3-4cm above the carina
- Check for a widened mediastinum
- Mass lesions (eg tumour, lymph nodes)
- Inflammation (eg mediastinitis, granulomatous inflammation)
- Trauma and dissection (eg haematoma, aneurysm of the major mediastinal vessels)
- B – Bones
- Check for fractures, dislocation, subluxation, osteoblastic or osteolytic lesions in clavicles, ribs, thoracic
- Spine and humerus including osteoarthritic changes
- At this time also check the soft tissues for subcutaneous air, foreign bodies and surgical clips
- Caution with nipple shadows, which may mimic intrapulmonary nodules
- compare side to side, if on both sides the “nodules” in question are in the same position, then they are likely to be due to nipple shadows
- C – Cardiac
- Check heart size and heart borders
- Appropriate or blunted
- Thin rim of air around the heart, think of pneumomediastinum
- Check aorta
- Widening, tortuosity, calcification
- Check heart valves
- Calcification, valve replacements
- Check SVC, IVC, azygos vein
- Widening, tortuosity
- D – Diaphragm
- Right hemidiaphragm
- Should be higher than the left
- If much higher, think of effusion, lobar collapse, diaphragmatic paralysis
- If you cannot see parts of the diaphragm, consider infiltrate or effusion
- If film is taken in erect or upright position you may see free air under the diaphragm if intra-abdominal perforation is present
- E – Effusion
- Effusions
- Look for blunting of the costophrenic angle
- Identify the major fissures, if you can see them more obvious than usual, then this could mean that fluid is tracking along the fissure
- Check out the pleura
- Thickening, loculations, calcifications and pneumothorax
- F – Fields (Lungfields)
- Check for infiltrates
- Identify the location of infiltrates by use of known radiological phenomena, eg loss of heart borders or of the contour of the diaphragm
- Remember that right middle lobe abuts the heart, but the right lower lobe does not
- The lingula abuts the left side of the heart
- Identify the pattern of infiltration
- Interstitial pattern (reticular) versus alveolar (patchy or nodular) pattern
- Lobar collapse
- Look for air bronchograms, tram tracking, nodules, Kerley B lines
- Pay attention to the apices
- Check for granulomas, tumour and pneumothorax
- G – Gastric Air Bubble
- Check correct position
- Beware of hiatus hernia
- Look for fee air
- Look for bowel loops between diaphragm and liver
- H – Hilum
- Check the position and size bilaterally
- Enlarged lymph nodes
- Calcified nodules
- Mass lesions
- Pulmonary arteries, if greater than 1.5cm think about possible causes of enlargement
R Middle Lobar PNA

Mikael Häggström, M.D. , CC0, via Wikimedia Commons
R Influenza PNA patch consolidations

Mikael Häggström, M.D., CC0, via Wikimedia Commons
Tuberculosis

Unknown author, Public domain, via Wikimedia Commons
Ultrasound
[table id=8 /]


Fetus heartbeat
Marcel Berteler / Public domain
CT
[table id=9 /]
MRI
[table id=10 /]



