The Ophthalmology section provides the most common eyed disorders tested in the USMLE, COMLEx, Medical School, and Residency. for Providing educational resources for students who are interested in the medical field, medical school, and medical professionals. Learn ahead and have fun.
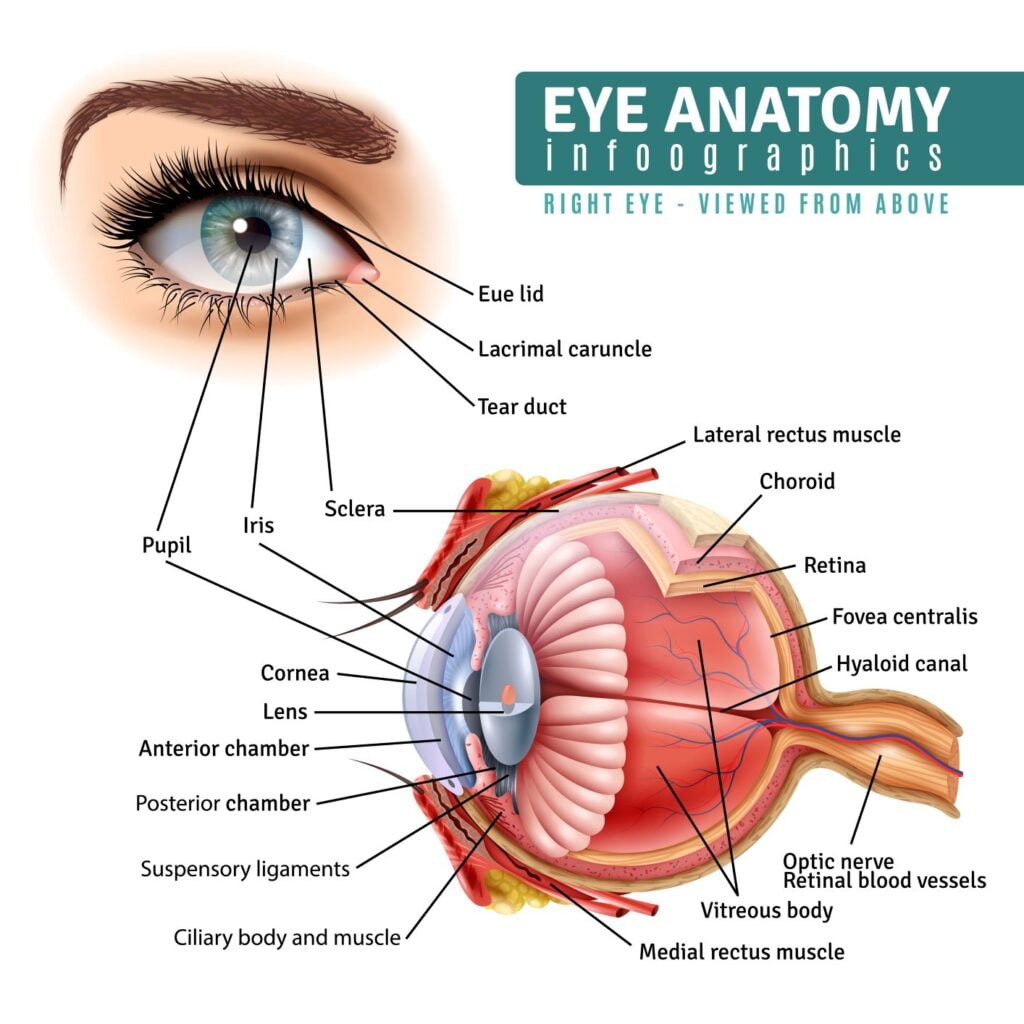
Eye Muscles
| Muscle | Function | Muscle | Function |
| Superior rectus | Elevation Intorsion Adduction CN3 – Superior | Inferior Rectus | Depression Extorsion Adduction CN3 – Inferior |
| Medial Rectus | Adduction of eye (CN3 – inferior) | Superior Oblique | Intorsion Depression Adduction CN4 |
| Lateral Rectus | Abduction of eye (CN 6) | Inferior Oblique | Extorsion Elevation Abduction CN3-Inferior |
Blepharitis
- Presentation:
- Burning, itching, excessive tearing, red/swollen eyelids, crusting/flaking, light sensitivity, blurred vision, +/- conjunctival infection
- Cause:
- Anterior: eyelashes (MC Seborrhea or S. aureus)
- Posterior: inner lid & meibomian glands (MC Rosacea or S. aureus)
- Management:
- Chronic disorder:
- Educate
- Warm compress, lid massage to express glands, lid washing
- Antibiotics:
- -Mild: topical azithro 1 %
- Severe:
- Oral antibiotics
- Chronic disorder:

clubtable / Public domain
Cataract
- Presentation:
- Painless, progressive, visual impairment, typically bilateral, poor night vision, difficulty reading fine print
- Cause:
- Opacity of the lens of the eye. Cataract Sx is the MC performed Sx in the US. Leading cause of blindness. MC >65 y/o.
- Acquired:
- from systemic dz (DM), Trauma, Toxic (Steroids)
Congenital: Hereditary, early embryonic (transplacental) damage (MC Rubella)
- from systemic dz (DM), Trauma, Toxic (Steroids)
- Risk:
- Increased risk: Ageing, Sun exposure, radiation exposure, smoking
- Management:
- Definitive: refer for surgery – Standard Extracapsular Cataract Extraction (ECCE)
- CI: uncontrolled glaucoma, macular degeneration
Rakesh Ahuja, MD, CC BY-SA 3.0, via Wikimedia Commons
Chalazion
- Presentation:
- Rubery, painless non tender nodular lesion that may distort vision if pressing on the cornea
- Cause:
- Obstruction of meibomian glad causing inflammation/lesion
May occur following a hordeleum
- Obstruction of meibomian glad causing inflammation/lesion
- Management:
- Warm compress, usually resolves in a few months
- Refer for Incision and Curettage if persistent
“File:Hordeolum.JPG” by Michal Klajban is licensed under CC BY-SA 3.0
Conjunctivitis
Bacterial Conjunctivitis
- Presentation:
- Unilateral, eyelids stuck together in the morning, not itchy, conjunctival swelling, mild photophobia, discomfort, mucopurulent discharge w/ yellow crusting,
- Lasts 10-14 days
- Cause:
- MC: S. aureus, Moraxella catarrhalis, H. Influenzae
- Management:
- Erythromycin Ointment or Trimethoprim-polymyxin B drops
IF Contacts: Ofloxacin to cover pseudomonas
- Erythromycin Ointment or Trimethoprim-polymyxin B drops
Viral Conjunctivitis
- Presentation:
- begins unilaterally and progresses to bilateral, itchy, fever, sore throat, foreign body sensation, watery discharge, cobblestoning palpebral conjunctiva,
Lasts 7-10 days
- begins unilaterally and progresses to bilateral, itchy, fever, sore throat, foreign body sensation, watery discharge, cobblestoning palpebral conjunctiva,
- Cause:
- MC: Adenovirus
- Management:
- Patient education (very contagious), cold compress, artificial tears (3-5 x day)
Corneal Abrasion
- Presentation:
- Severe Pain, photophobia, foreign body sensation
- Cause:
- Caused by traumatic events from foreign body or contact lenses
- Physical Exam:
- Assess: visual acuity loss, penlight – pupils, fundoscopic – confirm red reflex
- Diagnosis:
- Fluorescein Stain, do this after above exams to confirm diagnosis
- Management:
- Differentiate b/w abrasion & ulceration
 “File:Corneal Abrasion with Fluorescein Staining.jpg” by James Heilman, MD is licensed under CC BY-SA 4.0
“File:Corneal Abrasion with Fluorescein Staining.jpg” by James Heilman, MD is licensed under CC BY-SA 4.0
Corneal Ulcer
- Presentation:
- Pain, photophobia, tearing, decreased visual acuity, circumcorneal inje purulent or watery discharge
- Diagnosis:
- Fluorescein Stain
Dacryocystitis
- Presentation:
- Pain, tenderness, swelling, redness in the tear sac area or lacrimal gland area, purulent discharge
- If chronic: MC is mucopurulent drainage
- Cause:
- Congenital or acquired infection of the nasolacrimal system
- MC in infants & adults >40y/o
- Acute: S. aureus or GABHS
- Chronic: S. epidermidis or C. albicans
- Complications:
- Periorbital Infections & Sepsis
- Management:
- Congenital:
- usually resolves, but can do probe or nasolacrimal intubations
- Acute:
- Blood & drainage cultures, oral abx (IV if orbital cellulitis)
- Clindamycin and Vancomycin, +/- Sx
- Chronic:
- Topical Tobramycin 3 to 5 days,
- Dacryocysthrinostomy, +/- nasolacrimal intubation
- Congenital:
Ectropion
- Presentation:
- dry, painful eye with excessive tearing (epiphora), redness, chronic conjunctivitis, keratitis
- Cause:
- Turning out of edge of eyelid so inner surface is exposed
Causes: Facial palsy, Age, Scaring, Down’s syndrome
- Turning out of edge of eyelid so inner surface is exposed
- Complications:
- Corneal abrasions, ulcers, infections, light sensitivity, decreased vision
- Management:
- Artificial tears
- Symptomatic
- – tighten eyelid
Entropion
- Presentation:
- Decreased vision, excessive tearing/mucus, discomfort/pain, redness
- Cause:
- Turning in of edges of the eyelid (usually lower)
- Can be acquired or congenital
- Acquired: due to aging
- 1. dehiscence of lower-lid from the inferior tarsal border
- 2. horizontal lid laxity
- 3. enophthalmos
- Cicatricial: Scaring of palpebral/tarsal conjunctiva from Tacoma, chem burn, diseases or trauma
- Management:
- Artificial tears, tape eyelids
- Symptomatic
- – Botox A to paralyze orbicularis muscle
Glaucoma
Acute Angle-Closure Glaucoma
- Presentation:
- Emergency! Leads to permanent blindness
- Pain centered over eye
First episode - Rapid onset unilateral pain & pressure, blurred vision, seeing halos/photophobia, peripheral to central vision loss, pupillary dilation, steamy cornea, fixed pupil, red eye (conjunctival injection)
- Physical Exam:
- Red Eye
- Decreased visual acuity
- Diagnosis:
- IOP >21 & Cup to Disk >0.3
- Management:
- Timolol, Diamox, mannitol, laser iridotomy
Chronic Open Angle Glaucoma
- Presentation:
- usually asymptomatic & may be diagnosed accidentally during the exam. Slow, painless bilateral peripheral vision loss & poor night vision.
- Cause:
- MC types & characterized as chronic
- Diagnosis:
- Tonometry IOP >21, Cup to Disk >0.5
Exam: Cupping of the optic disc with thinning rim
- Tonometry IOP >21, Cup to Disk >0.5
- Management:
- 1st line beta-blockers (timolol)
- 2nd line: Prostaglandin analogs (Xalatan or Latanoprost)
- Laser trabeculoplasty or open Sx
Herpes Keratitis
| Presentation | Cause | Diagnosis | Management |
| Conjunctival injection/erythema, swollen, painful | Infection of the cornea | Fluorescein stain (dendritic pattern) | NEVER use steroids Acyclovir PO Topical trifluridine or idoxuridine (anti-herpetic) |
Hordeolum (Stye)
| Presentation | Cause | Diagnosis | Management |
| Painful, Purulent nodular lesion of eyelid | External: Abscess of hair follicle/external sebaceous gland Internal: Abscess of meibomian gland (seen when eyelid is inverted) MC acute bacterial (S. aureus) | 1st line Topical Abx: Bacitracin, tobramycin, erythromycin Warm Compress 2nd Line: Oral/IV Abx to prevent orbital cellulitis Incision & Drainage if no improvement in 48 hours |
Hyphema
| Presentation | Cause | Diagnosis | Management |
| Photophobia, >21 mmHg IOP, decreased visual acuity, corneal blood staining, enlarged/misshapen pupil | Blood in the anterior chamber following trauma or coagulopathy | Protection & Bed rest at 30 degrees Beta blocker or carbonic anhydrase inhibitor NEVER use NSAIDs Surgery |
Macular Degeneration
| Presentation | Cause | Diagnosis | Management |
| Gradual Bilateral loss of central vision, difficulty driving/reading | MCC of blindness in elderly in US | Amsler Grid Dry (10%): – Macular atrophic changes w/ ageing – Drusen (yellow retinal deposits) Wet (90%): – Neovascular changes cause macular degeneration – More rapid and severe | Dry: – Supportive: Vit A, C, E, Zinc and Beta Carotene Wet: – Intravitreal injections (ranibizumab, bevacizumab or aflibercept) – Anti-VEGF – Laser |
Optic Neuritis
| Presentation | Cause | Diagnosis | Management |
| Painful acute monocular vision loss, slow pupillary response | Acute inflammation & demyelination of the optic nerve MCC is MS | MRI to confirm demyelination | Methylprednisolone IV, Neuro eval |
Orbital Blow-out Fracture
| Presentation | Cause | Diagnosis | Management |
| protrusion or impingement of orbital fat, Diplopia, enophthalmos | Orbital fracture from trauma to eye globe or orbital rim Causes EOM entrapment and nerve damage –> paralysis of gums, upper lip, cheek | CT | Surgery w/in 10 days |
Orbital Cellulitis
| Presentation | Cause | Diagnosis | Management |
| decreased mobility, pain with eye movement, proptosis | Infection of the extraocular muscles & periorbital fat MC in younger children Polymycrombial infection MC Staph/Strep sp. may be fungal. Secondary to other infections: Sinusitis, orbital trauma, eye sx, dacryocystitis, tooth infection, facial infection, inner ear infection, mucocele | CT to confirm orbital involvement | Combo IV Abx Vanco + Ceftriaxone or Cefotaxime Ampicillin-sulbactam Piperacillin-tazobactam |
Periorbital Cellulitis
| Presentation | Cause | Diagnosis | Management |
| No visual changes, No pain with eye movement | Inflammation of eyelid and surrounding skin. More beningn than Orbital Cellulitis | CT to confirm orbital involvement | Combo IV Abx Vanco + Ceftriaxone or Cefotaxime Ampicillin-sulbactam Piperacillin-tazobactam |
Pinguecula
| Presentation | Cause | Diagnosis | Management |
| Benign growth, yellow color, does not grow onto the cornea |
Pterygium
| Presentation | Cause | Diagnosis | Management |
| Benign vascular corneal growth starting from nasal conjunctiva –> cornea. Triangular appearance | Artificial tears, Surgical removal if: – Obstructs vision, decreased eye movement, persistent irritation, cosmetic |
Retinal Artery Occlusion
| Presentation | Cause | Diagnosis | Management |
| Amaurosis Fugax, Sudden unilateral visual loss, cherry red macula, pale optic nerve | Acute occlusive disease of retinal artery, MCC is ruptured carotid plaque | 100% O2 therapy, ocular massage, acetazolamide (decrease ocular pressure), thrombolytic |
Retinal Vein Occlusion
| Presentation | Cause | Diagnosis | Management |
| Branch RVO: often asymptomatic Central RVO: Sudden blurry or loss of vision in one eye, “blood and thunder” appearance Hemi RVO | 2nd MCC of Retinopathy (after DM) | Ranibizumab, Intravitreal steroids, thrombolytics, Sx (Vitrectomy) |
Retinal Detachment
| Presentation | Cause | Diagnosis | Management |
| Painless visual field loss associated with location of detachment. Small: Floaters or flashing lights Large: “Curtain coming down” | Spontaneous: DM, extreme myopia Traumatic Tear or degradation of retina: DM, Retinopathy, vitreous invasion | w/o tear: Ophtho follow-up w/ tear: Sx reattachment, laser, cryotherapy, injection of expandable gas, sclera buckler |
Strabismus
| Presentation | Cause | Complications | Diagnosis | Management |
| Amblyopia (lazy eye) – Esotropia: eye turns towards nose – Exotropia: eye turns outward – Hypotropia: eye turns down – Hypertropia: eye turns up | Eyes move in different directions sending different images to the brain | Retinal detachment or Endophthalmitis | Glasses, surgery to achieve binocular vision & alignment |
Thrombosis of Cavernous Sinus
| Presentation | Cause | Diagnosis | Management |
| Same as orbital cellulitis plus Fever, Ptosis, Chemosis (conjunctival edema) & Palsy of any one of the involved CN, visual loss or diplopia, venous drainage may be impaired | Infection of the sphenoid sinus & internal carotid artery, CN III, IV, V & VI. Infection can spread to contralateral cavernous sinus & Intracranial. | Emergency Abx & Surgery of sinus |







